Best Wound Debridement Techniques for Effective Healing?
Wound debridement is a critical process in wound care. It involves removing dead or infected tissue to promote healing. Dr. Emily Thompson, a leading expert in wound care, emphasizes this point, stating, "Effective wound debridement is essential for optimal patient outcomes." This technique can significantly influence healing speed and reduce complications.
There are various debridement methods, each with unique benefits and challenges. For example, surgical debridement is highly effective but may require anesthesia. In contrast, enzymatic debridement is painless but takes longer to show results. Each method has its nuances that healthcare providers must navigate carefully.
Unfortunately, there are gaps in knowledge regarding the best practices for wound debridement. Some practitioners may rely on outdated techniques that are not evidence-based. More research is needed to refine methods and improve patient care in this field. Proper debridement techniques are vital for effective wound healing and better patient outcomes.
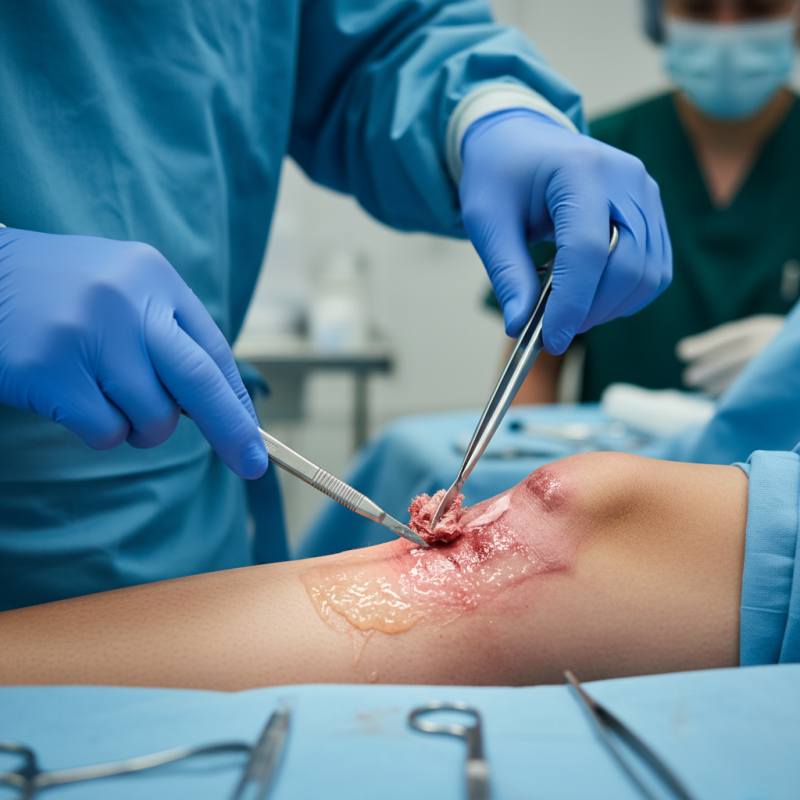
Overview of Wound Debridement and Its Importance in Healing

Wound debridement plays a crucial role in enhancing healing processes. It involves the removal of dead tissue, foreign materials, and potential pathogens from wounds. The objective is to create an environment conducive to healing. According to a report from the Wound Healing Society, effective debridement can reduce healing time by up to 50%. This statistic emphasizes the importance of timely wound management.
Different techniques are available for debridement, including autolytic, mechanical, and enzymatic methods. Autolytic debridement, for example, uses the body's own processes to break down dead tissue. This method is generally safe and can be performed with minimal resources. However, it may take longer than other techniques. Mechanical debridement, while faster, can cause discomfort. A study published in the Journal of Wound Care showed that mechanical removal effectively debrides 70% of necrotic tissue within the first session.
Understanding the type of wound is critical for choosing the right technique. Chronic wounds may need a more aggressive approach, while acute wounds can often heal with gentler methods. The choice contributes to wound healing efficiency. This complexity means that healthcare practitioners must evaluate each case carefully. A personalized approach can greatly enhance patient outcomes, addressing healing challenges during treatment.
Types of Wound Debridement Techniques: A Comprehensive Guide
Wound debridement is essential for promoting effective healing. Various techniques exist, each with unique benefits. Understanding these methods can significantly impact patient recovery.
Enzymatic debridement uses topical agents to dissolve necrotic tissue. It requires patience, as results can take time. This method is less painful but may not be suitable for all wounds. Always evaluate the specific wound characteristics before proceeding. In contrast, autolytic debridement relies on the body's own process, utilizing moisture-retentive dressings. It's gentle but may not be as quick or effective as other methods.
Each technique has its strengths and weaknesses. Debridement can be a balancing act. Understanding your options is key. Clear communication with patients about what to expect is crucial.
Indications and Contraindications for Each Debridement Method
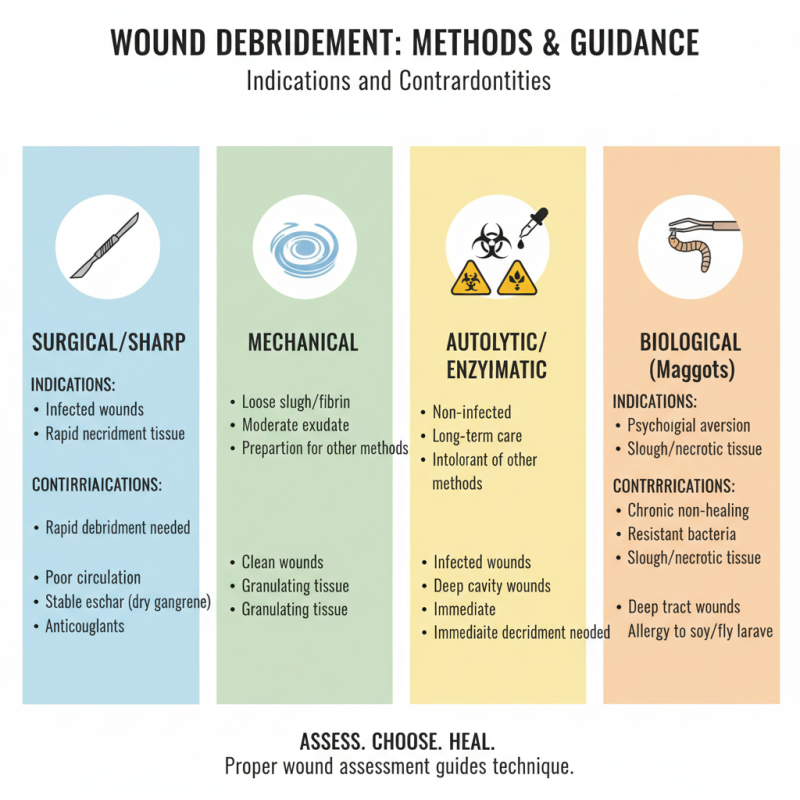
Wound debridement is a critical aspect of wound management. Each debridement method has specific indications and contraindications. Properly assessing the wound type guides the choice of technique, enhancing healing outcomes.
Surgical debridement is highly effective for deep or necrotic wounds. It removes dead tissue quickly. However, it requires skilled personnel and anesthesia, which may not be suitable for all patients. A study published in the Journal of Wound Care indicates that surgical debridement leads to an 85% healing rate in chronic wounds. Yet, the risk of infection increases if proper sterile techniques are not utilized.
Autolytic debridement utilizes the body's natural processes to remove necrotic tissue. It is typically indicated for superficial wounds without heavy exudate. While safe and patient-friendly, it may take longer to achieve desired results. In some cases, patients may find it inadequate for larger wounds. Data show that autolytic methods may be slower, with healing rates around 50% after four weeks. This underlines the need for careful patient selection and ongoing assessment of wound progress.
Post-Debridement Care: Ensuring Optimal Healing Environment
Post-debridement care is crucial for ensuring that wounds heal effectively. Research indicates that a suitable environment greatly enhances healing rates. A study from the Journal of Wound Care reported that optimal moisture levels in the wound bed can accelerate healing by nearly 50%. This highlights the importance of maintaining a balanced wound environment.
Following debridement, clinicians often recommend using advanced dressings. These dressings help to maintain moisture while providing a barrier against infection. Infection rates can rise significantly if the wound is not adequately protected. According to the American College of Surgeons, untreated wounds can lead to complications, increasing healing time by 30%.
It’s vital to monitor the progress of the wound. Regular assessments can reveal signs of infection or delayed healing. A 2021 report showed that timely intervention when complications arise could reduce healing time by 25%. Engaging with patients about their wound care routine promotes better outcomes. As healthcare providers, reflecting on our practices can improve patient experiences and healing outcomes.
Best Wound Debridement Techniques for Effective Healing - Post-Debridement Care: Ensuring Optimal Healing Environment
| Technique | Description | Indications | Post-Debridement Care |
|---|---|---|---|
| Surgical Debridement | Removal of devitalized tissue using surgical instruments. | Severe wounds with necrotic tissue. | Monitor for infection, maintain a moist environment. |
| Mechanical Debridement | Utilizes pressure irrigation or wet-to-dry dressings. | Chronic wounds with a buildup of debris. | Ensure dressing changes are done regularly. |
| Chemical Debridement | Application of topical agents that digest dead tissue. | Wounds where surgical options pose high risks. | Follow specific agent instructions for safety. |
| Autolytic Debridement | Uses the body's own mechanisms to remove dead tissue. | Less severe and stable wounds. | Maintain a moist environment, check regularly for progress. |
| Bio-debridement | Uses larvae to consume necrotic tissue. | Chronic and complex wounds. | Protect surrounding skin and ensure a sterile environment. |
Future Trends and Innovations in Wound Debridement Techniques
The field of wound debridement is evolving rapidly. New techniques are emerging to improve healing outcomes. One promising trend is the use of bioengineered materials. These materials are designed to mimic natural skin properties. They provide a beneficial environment for healing. By promoting cell growth, they enhance the body's natural repair processes.
Another innovation includes advanced ultrasound technology. Studies suggest that this method can enhance the debridement process. It allows for precise removal of necrotic tissue without harming surrounding healthy areas. Such techniques require further research but show potential for future applications.
Telemedicine is also on the rise in wound care. It allows healthcare professionals to monitor wound healing remotely. Patients receive timely advice, which can improve healing rates. However, the reliance on technology raises some challenges. Ensuring access to devices remains a concern, especially in underserved areas. The future of wound debridement will be shaped by these advancements, making healing more effective and accessible for all.
Best Wound Debridement Techniques for Effective Healing
Related Posts
-

Essential Wound Debridement Checklist for Effective Patient Care
-

How to Choose the Right Wound Dressing for Effective Healing Solutions
-

Top 10 Wound Care Supply Manufacturers from China at the 137th Canton Fair
-
Finding Top Suppliers for Best Wound Cleansing Solutions in the Global Market
-

Why Effective Wound Debridement Products Are Essential for Faster Healing Rates
-

Understanding the Importance of Quality Wound Care Supplies for Effective Healing
